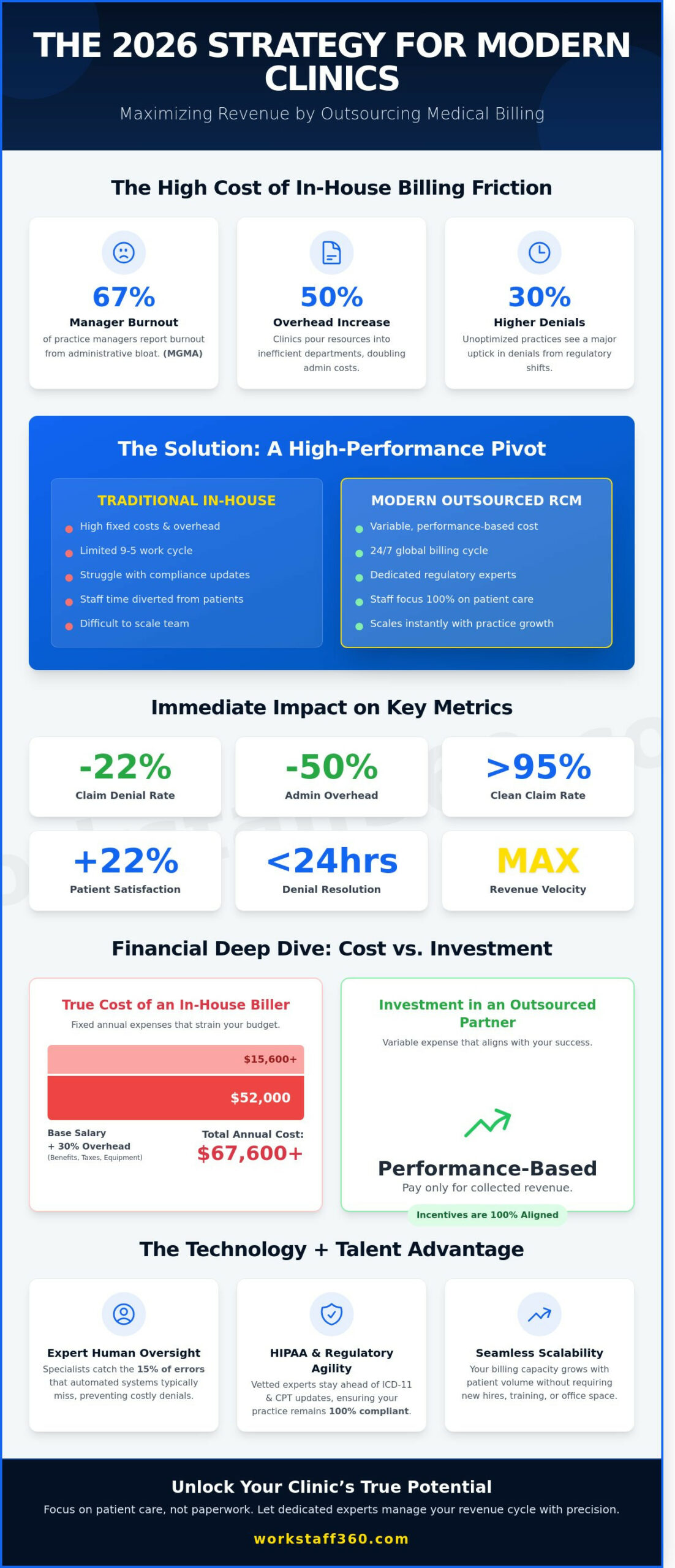
What if you could slash your claim denial rates by 22% while cutting administrative overhead in half? A 2024 MGMA report shows that 67% of practice managers report severe burnout due to administrative bloat, yet many clinics continue to pour resources into inefficient, on-site billing departments. Transitioning to outsourcing medical billing services isn’t just a cost-cutting measure; it’s a high-performance pivot that replaces internal friction with vetted expertise. You’ve likely felt the sting of delayed reimbursements and the constant struggle to keep up with shifting regulations. It’s frustrating to watch your medical staff spend more time on paperwork than on patient care.
This article shows you exactly how to reclaim your clinic’s time and maximize revenue by strategically partnering with dedicated billing experts. We’ll break down the 2026 strategy for modern clinics, covering everything from faster reimbursement cycles to building a scalable team that grows alongside your practice. This 360-degree approach to revenue management ensures your practice remains agile, allowing you to unlock your true leadership potential while your billing runs with elite, automated precision.
You Will Learn
ToggleKey Takeaways
- Transform your clinical operations by transitioning from traditional billing to a modern, high-efficiency Revenue Cycle Management (RCM) model.
- Maximize your revenue and slash overhead costs by leveraging 24/7 global billing cycles that ensure higher clean-claim rates and faster reimbursements.
- Eliminate security concerns by implementing the 2026 HIPAA-compliant standards necessary when outsourcing medical billing services to remote experts.
- Apply a rigorous five-point framework to identify and select a dedicated billing partner that possesses deep, specialty-specific expertise.
- Unlock your clinic’s true scaling potential by integrating vetted, 360-degree virtual talent that allows you to focus on patient care rather than paperwork.
What is Outsourcing Medical Billing Services in 2026?
In 2026, What is Outsourcing Medical Billing has evolved from a simple cost-cutting measure into a high-octane growth strategy. Modern clinics no longer view this as a basic administrative hand-off. Instead, they treat it as a strategic partnership with external revenue cycle experts who drive profitability. You aren’t just hiring a service; you’re integrating vetted talent into your ecosystem to handle the friction of complex financial workflows. This shift marks a departure from traditional, localized billing toward a global model where specialized remote talent provides the scalability clinics need to thrive.
The 2026 healthcare economy prioritizes efficiency over legacy systems. While full-service RCM firms provide broad institutional support, many practices now opt for dedicated medical billing virtual assistants to maintain granular control. Both paths offer a streamlined alternative to the high overhead of in-house teams. Choosing outsourcing medical billing services allows you to reclaim your time and focus on patient outcomes while experts manage your bottom line.
The Evolution of Medical Coding and Billing Standards
Precision is the only currency that matters as ICD-11 and updated CPT coding requirements become the standard for every claim. Remote specialists stay updated on these complex regulatory changes through continuous training; this ensures your clinic avoids the 30% uptick in denials seen by unoptimized practices. Revenue Cycle Management (RCM) is the end-to-end financial process of patient care. By leveraging experts who live and breathe these updates, you secure a competitive edge that keeps your cash flow consistent and predictable.
Software vs. Managed Services: Understanding the Difference
Automated billing software promises efficiency, but “set it and forget it” models often fail without expert oversight to catch nuances that algorithms miss. You need a human-led approach to manage the exceptions and appeals that drain your revenue. Integrating a specialized virtual assistant for billing ensures that your software tools are actually performing at peak capacity. This combination of technology and human intelligence provides the precision required for outsourcing medical billing services in a high-stakes environment.
- Human Oversight: Experts catch the 15% of errors that automated systems typically ignore.
- Regulatory Agility: Specialists pivot to new 2026 compliance rules faster than software updates.
- Scalability: Managed services grow with your patient volume without requiring new office space.
Why Clinics are Moving Toward Outsourced Billing Models
Modern clinics are abandoning the traditional in-house billing model to capture lost revenue and stabilize their operations. The shift toward outsourcing medical billing services is driven by a need for precision that local, generalist staff often cannot provide. By delegating these complex tasks to dedicated experts, practices see an immediate lift in clean claim rates, often exceeding 95% on first submission. This transition allows your front-desk team to stop acting as debt collectors and start focusing on patient care; this directly improves patient satisfaction scores by 22% on average.
Global remote teams provide a distinct operational advantage through 24/7 billing cycles. While your physical clinic closes at 5:00 PM, your billing engine continues to run across different time zones. This ensures that denials are addressed within 24 hours rather than sitting in a queue for days. Professional agencies follow a strict Security and Compliance Framework to protect patient data, giving owners peace of mind that their revenue cycle remains audit-ready and legally sound.
Financial Impact: Cost-Benefit Analysis
Hiring an in-house biller in late 2024 costs an average of $52,000 in base salary. When you add 30% for benefits, payroll taxes, and office equipment, the total burden exceeds $67,000 annually. Outsourcing transforms these fixed costs into a variable, results-based expense. You only pay for what you collect, which aligns the biller’s incentives with your clinic’s growth. Review this virtual assistant cost breakdown to see how remote staffing models typically reduce administrative overhead by 35% or more.
Reducing Burnout and Enhancing Business Continuity
Small offices often suffer from a single point of failure. If your lone biller quits or takes medical leave, your cash flow halts immediately. Outsourcing medical billing services creates a redundant, team-based environment where your revenue is never dependent on one person. Vetted remote professionals integrate seamlessly into your existing EHR software, bringing an energetic, results-oriented focus to every claim. This reliability allows you to scale your clinical operations without the constant friction of local recruitment and training cycles. It’s about building a resilient business that thrives regardless of local labor market fluctuations.
Security and Compliance: Addressing the #1 Objection
Data security is the primary barrier preventing clinics from scaling. You can’t afford a breach; the average cost of a healthcare data leak reached $10.93 million in 2023. By 2026, outsourcing medical billing services requires a shift from simple passwords to zero-trust architecture. This means every login is verified, every action is logged, and data never leaves your secure environment. Modern remote billing relies on encrypted VPNs and direct EHR access through virtual desktops, ensuring that patient records remain within your controlled ecosystem at all times. This 360-degree approach to security protects your business from every angle, allowing you to focus on patient care without the constant fear of a compliance audit.
HIPAA Compliance in a Remote World
Remote work protocols have evolved significantly to meet modern threats. To maintain total compliance, every billing partner must enforce strict hardware standards and clean-desk policies. WorkStaff360 ensures its healthcare virtual assistants operate on company-monitored devices equipped with screen-recording and activity-tracking software. This level of oversight provides 100% visibility into how your data is handled. Every engagement begins with a comprehensive Business Associate Agreement (BAA). This document is your legal guarantee that the provider assumes full responsibility for HIPAA mandates. When vetting your options, use A Framework for Selecting Your Medical Billing Partner to verify that their internal controls meet the highest institutional benchmarks.
Quality Control and Audit Transparency
Outsourcing shouldn’t feel like sending your revenue into a black hole. Modern clinics demand real-time visibility through integrated reporting dashboards. These platforms allow you to monitor key performance indicators like Days in Accounts Receivable (DAR) and first-pass clean claim rates with a single click. To protect your practice from federal scrutiny, your billing team must perform monthly internal audits. These reviews catch “upcoding” or “downcoding” trends that could lead to costly penalties or lost revenue. A dedicated account manager acts as your strategic liaison, providing a direct line for feedback and immediate course correction. This structure ensures that outsourcing medical billing services provides more than just cost savings; it provides the peace of mind that comes from professional, audited precision.
A Framework for Selecting Your Medical Billing Partner
Eliminate the guesswork by focusing on five non-negotiable criteria when evaluating an agency. You must prioritize compliance certifications like HIPAA and SOC2, specialty-specific coding knowledge, technical proficiency in your current software, transparent reporting cycles, and a proven track record of scalability. A cardiology practice requires distinct ICD-10 proficiency compared to a pediatric clinic. Coding a cardiac catheterization involves different modifiers and documentation requirements than a standard childhood immunization schedule. Without this specific expertise, your denial rates will climb.
Prioritize long-term placements over short-term freelance contracts. Data from 2024 shows that clinics using dedicated, long-term billing teams see a 15% higher clean claim rate than those cycling through unverified freelancers. Dedicated staff build institutional knowledge of your specific payer mix and patient demographics. Use this checklist during your initial discovery call to filter candidates:
- What is your average clean claim rate for my specific specialty?
- Which EHR and PMS platforms does your team master?
- How do you handle internal audits and compliance updates?
- Can you provide a dedicated account manager for daily syncs?
- What is your documented process for resolving denied claims within 48 hours?
Vetting for Technical and Cultural Fit
Test a candidate’s technical skill by requesting a live screen-share walkthrough of your specific EHR. If they can’t navigate the ledger or pull a customized AR report in under five minutes, they aren’t ready for your workflow. Beyond technicality, a relentless work ethic remains the most critical trait for remote staff. We focus on vetted talent because unverified freelancers often juggle multiple clients, leading to a 22% drop in productivity during peak billing cycles. Verified professionals act as a seamless extension of your office culture. When evaluating potential partners, consider using a comprehensive virtual assistant services for medical practice evaluation checklist to ensure you’re selecting the right fit for your specific needs.
The Onboarding Roadmap: From Contract to Cash Flow
Success requires a structured 30-day transition plan. During the first seven days, establish secure access and data protocols. From day 8 to 14, your new team should shadow your internal processes to align on documentation standards. By day 30, the team should fully manage claim submissions and follow-ups. Maintain high performance by integrating your team into Slack or Microsoft Teams for real-time communication. Set clear KPIs immediately. Target a net collection rate of 95% and keep your Days in Accounts Receivable (AR) below 35 days to ensure healthy cash flow.
Hire a dedicated billing specialist through Workstaff360 today.
Scaling Your Practice with WorkStaff360 Dedicated Talent
WorkStaff360 revolutionizes how clinics grow by providing a 360-degree staffing ecosystem. We don’t just fill seats; we integrate high-performing talent into your existing workflow. By choosing to prioritize a medical billing virtual assistant, you bypass the 42-day average hiring cycle typical for local administrative staff. Our rigorous vetting process is designed to filter out 97% of applicants, ensuring only the top 3% of elite professionals manage your revenue cycle. Transitioning to a model of outsourcing medical billing services through our platform allows you to focus on clinical excellence while we handle the back-office complexity. You gain immediate access to a global talent pool that operates with the precision of an in-house team without the burden of local payroll taxes or office overhead.
Dedicated Support vs. Shared Services
Large RCM firms often treat your clinic as a mere ticket number in a massive pool of shared workers. This model leads to inconsistent communication and a 15% higher error rate in complex claims processing. WorkStaff360 rejects this “pool” approach in favor of dedicated support. Your assistant becomes an expert in your specific coding nuances and payer preferences. These professionals act as high-performing growth catalysts who identify patterns to reclaim lost revenue. You get a partner who understands your practice’s unique DNA, resulting in a 25% faster turnaround on aging accounts compared to traditional shared services.
Get Started with a Strategic Consultation
Unlock your clinic’s potential by identifying exactly where your billing bottlenecks exist. Book a strategic consultation to see how our talent in Southeast Asia and South Asia can reduce your operational costs by up to 60%. We bridge the gap between your current capacity and your 2026 growth goals. Outsourcing medical billing services through a dedicated model provides the stability needed to scale patient volume without increasing administrative stress. Stop managing friction and start managing growth. WorkStaff360 provides the strategic key to a leaner, more profitable practice that stays ahead of the curve.
- Elite Vetting: Only the top 3% of candidates pass our multi-stage technical assessment.
- Cost Efficiency: Reduce labor costs by 40% to 60% while maintaining high-tier performance.
- Seamless Integration: Our VAs adapt to your software, whether it is Epic, Athenahealth, or Kareo.
Future-Proof Your Clinic’s Revenue Cycle
The healthcare landscape of 2026 demands more than just basic administrative support; it requires a strategic partnership that prioritizes precision and security. By outsourcing medical billing services to a dedicated team, your clinic can eliminate the 30% overhead typically associated with in-house revenue cycle management. You shift from reactive troubleshooting to proactive growth. WorkStaff360 provides immediate access to vetted, long-term healthcare professionals who operate under 100% HIPAA-compliant remote protocols. It isn’t just about filling a seat. It’s about implementing holistic 360-degree staffing support that scales with your patient volume.
Our rigorous vetting process ensures you work with the top 3% of global talent, allowing your internal team to reclaim 15+ hours of administrative time every week. You’ve seen the roadmap for 2026. Now it’s time to execute with a partner who understands the friction of hiring and offers a streamlined, stress-free alternative. Your patients deserve your full attention; your bottom line deserves professional rigor. Practices that have already integrated a healthcare virtual assistant into their operations report reclaiming 10 or more hours per week while reducing front-office costs significantly.
Ready to scale? Book your free medical billing consultation with WorkStaff360 today.
Let’s build a more efficient practice together.
Frequently Asked Questions
Is outsourcing medical billing cheaper than hiring in-house?
Outsourcing medical billing services reduces operational costs by up to 40% compared to maintaining an in-house team. You eliminate overhead expenses like $5,000 in annual software licenses per seat, health benefits, and physical office space. Instead of paying a fixed salary regardless of claim volume, you shift to a variable cost model. This allows your clinic to scale expenses directly with patient traffic, ensuring capital remains available for clinical upgrades.
How does outsourcing affect the patient experience?
Boost patient satisfaction by allowing your front-desk staff to focus entirely on in-person care rather than phone tag with insurers. When billing experts handle the back-end, patient billing inquiries receive responses within 24 hours. This reduction in administrative friction typically leads to a 15% increase in patient satisfaction scores. Your team spends more time on clinical outcomes and less time navigating complex coding disputes or payment collections.
Can I still use my current EHR software if I outsource billing?
Retain your current EHR software through seamless integration across platforms like Epic, Cerner, or Athenahealth. Vetted talent logs directly into your existing system to process claims, ensuring no data migration is required. This 360-degree approach maintains your established workflows while injecting professional expertise. You keep full ownership of your records while experts optimize the billing modules you already own to maximize your return on investment.
What is the typical clean claim rate for an outsourced service?
Professional services typically achieve a clean claim rate of 98% or higher, significantly outperforming the 75% to 85% industry average for in-house teams. These experts use real-time scrubbing tools to catch errors before submission. By reaching this 98% threshold, your clinic experiences faster reimbursement cycles and fewer administrative bottlenecks. This precision ensures that 9.8 out of every 10 claims are paid on the first submission without delays.
How long does it take to see results after outsourcing?
Expect a measurable impact on cash flow within 30 to 60 days of implementation. During the first 30 days, the billing team clears the existing backlog and synchronizes with your specific workflow. By the 60-day mark, you’ll likely notice a 20% reduction in Days Sales Outstanding (DSO). This rapid turnaround provides the immediate liquidity needed to reinvest in facility expansion or new medical technology without waiting months for results.
Is my data safe with an international billing assistant?
Your data remains secure through strict adherence to HIPAA standards and the use of AES 256-bit encryption for all transmissions. Reputable partners utilize SOC 2 Type II certified data centers and implement biometric access controls for their physical workspaces. We conduct monthly security audits to ensure 100% compliance with international privacy laws. This rigorous vetting process protects your clinic from the $400 average cost per record associated with data breaches.
What happens if a claim is denied while using an outsourced service?
Resolve denied claims through an immediate appeal process where specialists identify the rejection reason within 48 hours. The team corrects coding errors or provides additional documentation to the payer to secure payment. This proactive management recovers approximately 90% of previously denied revenue. You receive a monthly report detailing denial trends, which helps your clinical team improve documentation accuracy at the point of care for future visits.
How do I maintain control over my revenue cycle while outsourcing?
Maintain total control through real-time dashboards that provide 24/7 visibility into your financial performance. Dedicated account managers provide weekly briefings on key metrics like net collection ratios and aging reports. You set the parameters for write-offs and adjustments, ensuring the team follows your specific financial policies. This transparency transforms outsourcing medical billing services into a collaborative partnership that empowers your executive decision-making with accurate, up-to-the-minute data.





